Epilepsy: A Continuous Condition, Monitored Episodically
Epilepsy is a lifelong neurological condition that unfolds across daily life, not just during clinical encounters. The current standard of care offers only partial visibility into a condition that is inherently continuous.
The Burden of Epilepsy
50M
Global Epilepsy Patients
3.4M
U.S. Epilepsy Patients
1.3M
Annual ER Visits due to Epilepsy
1.2M
Adults with Uncontrolled Epilepsy
1.3M
Annual Epilepsy Health Expenditure
Epilepsy affects 50 million people worldwide and imposes a substantial clinical, personal, and economic burden.
In the US alone, 3.4 million individuals require ongoing neurological care, with a significant proportion experiencing seizures that remain uncontrolled despite treatment. Epilepsy-related emergency visits and long-term healthcare costs reflect not only the severity of the condition but also the challenges of managing it over time.
This burden underscores the need for sustained clinical insight into how seizures occur and evolve in everyday life.
The Clinical Reality of Epilepsy Care
A Condition defined by Variability
Seizure frequency, type, and severity vary widely across patients and within individuals over time. Clinical management, therefore, depends on ongoing judgment rather than one-time assessment.
Despite advances in treatment, many care decisions are still made with limited objective insight into how seizures unfold outside the clinic, where most events actually occur.
Episodic Measurement in a Continuous Disease
EEG remains the clinical gold standard for assessing brain activity. In practice, however, EEG is most often captured during short, time-limited recordings.
These recordings provide valuable information, but they represent brief snapshots of a condition that evolves continuously across days, nights, and contexts. For patients with infrequent, variable, or context-dependent seizures, episodic measurement can miss meaningful patterns that only emerge over time.


What Happens Between Visits?
Most seizures occur outside controlled clinical environments, during daily life and sleep. As a result, clinicians must often rely on patient and caregiver reporting to understand what happens between appointments.
While essential, retrospective reporting has inherent limitations. Some events may go unnoticed, others may be difficult to characterize, and recall may be incomplete or imprecise. Together, these factors constrain visibility into the full clinical picture.
Partial Data, Complex Decisions
When objective data are sparse, assessing treatment response becomes difficult. Medication adjustments and care decisions may be guided by partial information, extending trial-and-error cycles for many patients.
Over time, this uncertainty can delay stabilization and increase burden for clinicians, patients, and families alike.


Mismatch Between Condition and Measurement
These limitations are not the result of inadequate clinical expertise or effort. They reflect a structural mismatch between how epilepsy behaves in real life and how it is typically measured.
The tools available today are optimized for episodic assessment, while the condition itself is continuous.
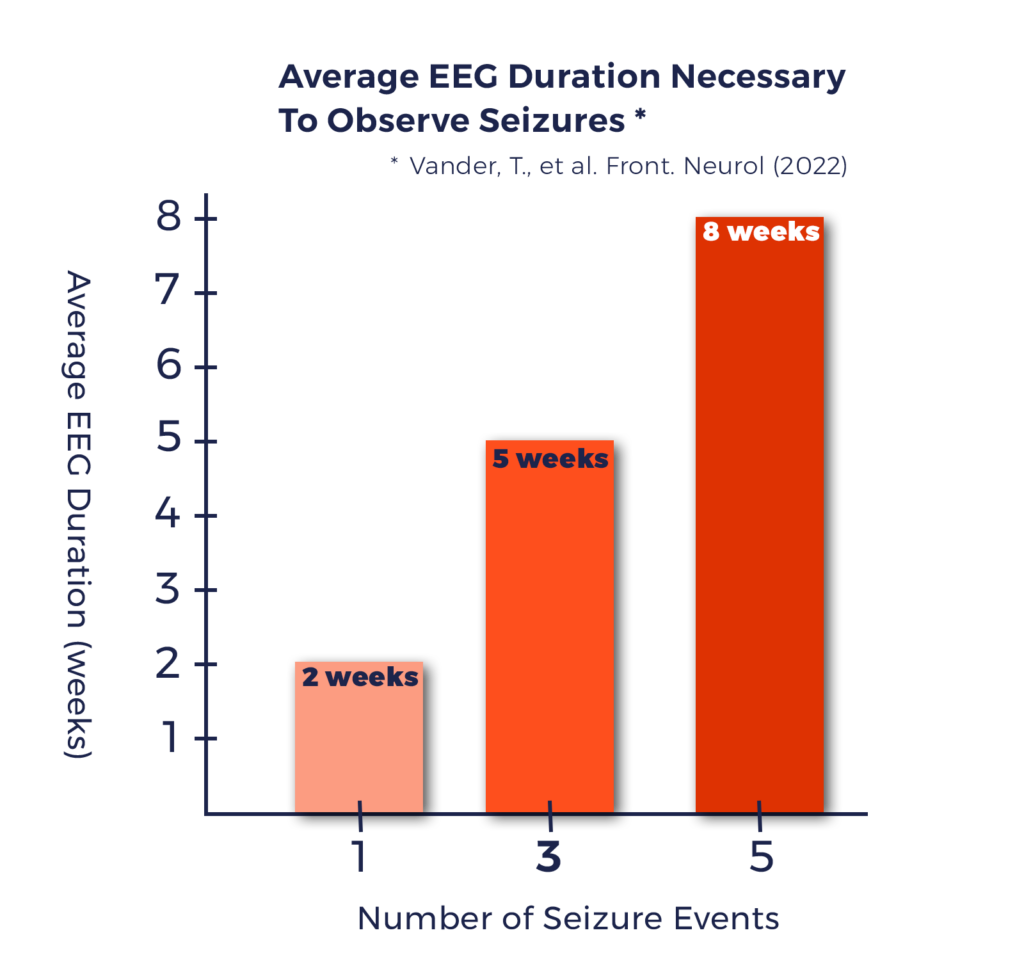
Why this Matters
Improving epilepsy care requires approaches that better align neurological monitoring with the lived reality of the condition. Recognizing this gap is foundational to advancing how seizure burden, treatment response, and long-term trajectories are understood.
This challenge sets the stage for rethinking how neurological insight is generated—supporting clinical judgment with a more complete view of patients’ daily lives.
